
If you’ve ever been told that painful periods are “just part of being a woman,” you’re not alone. For millions of people worldwide, that pain isn’t normal—it’s a sign of endometriosis, a chronic condition that affects an estimated 1 in 10 women and many transgender and non-binary individuals. Yet, despite how common it is, endometriosis remains widely misunderstood, underdiagnosed, and overlooked.
March is National Endometriosis Awareness Month, a time dedicated to shedding light on this painful and often invisible condition. Many people suffer in silence, dismissed by doctors, teachers, employers, and even loved ones who don’t realize just how debilitating endometriosis can be. On average, it takes 7 to 10 years for someone to receive a proper diagnosis, leaving many struggling with severe pain, fatigue, and infertility without answers.
Raising awareness isn’t just about sharing facts—it’s about changing the conversation. It’s about empowering those affected to advocate for themselves, pushing for better research, and making sure no one has to suffer in silence. In this post, we’ll dive into what endometriosis is, why it’s so difficult to diagnose, available treatment options, and how we can all help support those living with this condition.
What is Endometriosis?
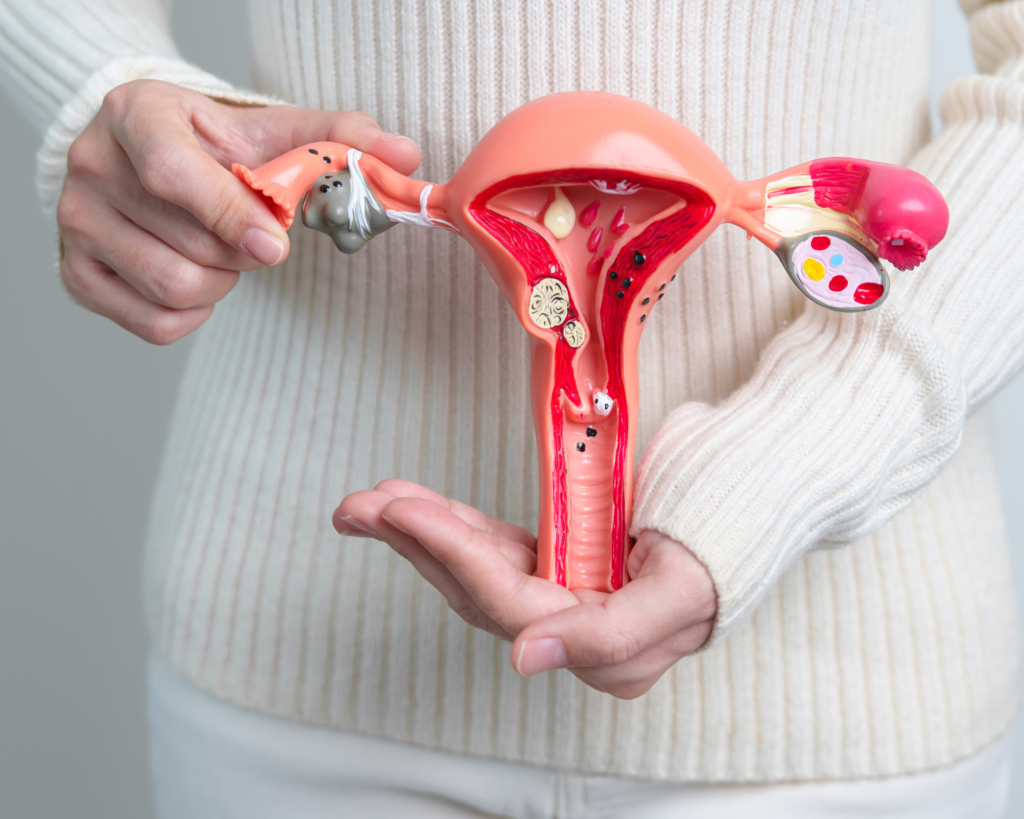
Endometriosis is a chronic and often painful condition that occurs when tissue similar to the lining of the uterus (endometrial tissue) grows outside the uterus. This misplaced tissue can be found on the ovaries, fallopian tubes, outer surface of the uterus, intestines, and even in more distant areas like the lungs in rare cases.
Much like the uterine lining, this tissue thickens, breaks down, and bleeds during each menstrual cycle. However, because it’s outside the uterus, it has nowhere to go. This can lead to inflammation, scarring, and painful adhesions that cause organs to stick together.
Common Symptoms of Endometriosis
The symptoms of endometriosis can vary widely from person to person, but some of the most common include:
- Severe pelvic pain – particularly during menstruation, but also before or after a period.
- Painful periods (dysmenorrhea) – cramps that are more intense and last longer than normal.
- Chronic lower back and abdominal pain – which may not be tied to the menstrual cycle.
- Pain during or after sex – caused by deep infiltrating endometriosis in the pelvic region.
- Painful bowel movements or urination – especially during a period.
- Heavy menstrual bleeding – including prolonged periods or spotting between cycles.
- Bloating and digestive issues (endo belly) – often mistaken for IBS.
- Fatigue – even without significant physical exertion.
- Infertility – in many cases, endometriosis is discovered when someone struggles to conceive.
Some individuals have mild endometriosis with severe symptoms, while others have severe cases with little to no symptoms, making diagnosis even more challenging.
Who is Affected?
Endometriosis primarily affects people assigned female at birth, including women, transgender men, and non-binary individuals. It can develop as early as a person’s first period and persist beyond menopause in some cases.
Despite its prevalence—impacting an estimated 200 million people worldwide—endometriosis is frequently dismissed as “bad period pain” or misdiagnosed as conditions like IBS, ovarian cysts, or pelvic inflammatory disease. The lack of awareness and research has left many struggling for answers and proper medical care.
Understanding what endometriosis is and who it affects is the first step in advocating for earlier diagnosis, better treatment options, and improved quality of life for those living with this condition.
The Challenges of Diagnosis
For many individuals with endometriosis, the road to diagnosis is long, frustrating, and filled with medical gaslighting. On average, it takes 7 to 10 years for someone to receive a proper diagnosis—a delay that can lead to years of unnecessary pain, complications, and even fertility struggles. But why does it take so long?
Why is Endometriosis So Often Misdiagnosed?
One of the biggest reasons endometriosis remains undiagnosed for so long is that its symptoms overlap with other conditions. Many individuals are told they have:
- Irritable Bowel Syndrome (IBS) – because of digestive issues like bloating, constipation, or diarrhea.
- Pelvic Inflammatory Disease (PID) – due to chronic pelvic pain.
- Ovarian cysts – since endometriosis can cause growths called endometriomas on the ovaries.
- Painful periods (dysmenorrhea) – often brushed off as “normal” menstrual cramps.
Another issue is that many healthcare providers aren’t properly trained to recognize endometriosis symptoms. Since pelvic pain is common among menstruating individuals, some doctors minimize the severity or misattribute it to stress, anxiety, or simply “being a woman.” Some people are even told they are overreacting or that the pain is “all in their head.”
Making things even more complicated, the only definitive way to diagnose endometriosis is through a laparoscopy—a surgical procedure that allows doctors to look inside the abdomen. Because of this, many people are put on birth control or pain medication as a temporary solution without ever getting a confirmed diagnosis.
The Toll of Delayed Diagnosis
The delay in diagnosis isn’t just frustrating—it’s physically, emotionally, and mentally draining. Many people spend years searching for answers, bouncing between doctors, undergoing unnecessary tests, and trying treatments that don’t work. The pain can interfere with school, work, relationships, and everyday life, leaving many feeling isolated, unheard, and hopeless.
💬 “For years, I was told my cramps were normal. I collapsed in pain at school, I missed work, I couldn’t even sit through a movie without discomfort. Doctors dismissed me over and over. It took almost 10 years before I finally got diagnosed with endometriosis, and by then, it had already caused severe damage.” – Anonymous
For those trying to conceive, the diagnosis can be even more devastating. Up to 50% of people with infertility issues are later diagnosed with endometriosis, often realizing that earlier intervention could have helped.
The sooner endometriosis is diagnosed, the better the chances of managing symptoms and preventing complications. National Endometriosis Awareness Month is an opportunity to spread the message that severe pain is not normal—and that no one should have to suffer in silence.
Treatment and Management Options for Endometriosis
There is no one-size-fits-all treatment for endometriosis, and unfortunately, there is no cure. However, a combination of medical treatments, lifestyle adjustments, and alternative therapies can help manage symptoms and improve quality of life. Since endometriosis affects individuals differently, treatment must be highly individualized—what works for one person may not work for another.
Medical Treatments for Endometriosis
For many individuals, the first step in managing endometriosis symptoms involves medical intervention. Some of the most common treatments include:
Pain Relievers – Over-the-counter NSAIDs like ibuprofen (Advil) or naproxen (Aleve) can help reduce inflammation and ease pain, but they are often not enough for severe cases.
Hormonal Therapies –
- Birth control pills, patches, or rings – These regulate hormones and can reduce pain by thinning the uterine lining.
- Progestin-only treatments (IUDs, injections, or pills) – These suppress ovulation and slow the growth of endometrial-like tissue.
- Gonadotropin-releasing hormone (GnRH) agonists – These create a temporary menopause-like state by lowering estrogen levels, but they come with side effects like bone density loss and mood changes.
Surgical Options –
- Laparoscopic excision surgery – The most effective way to remove endometriosis lesions while preserving fertility.
- Hysterectomy (removal of the uterus) – Sometimes recommended in severe cases, but it is not a guaranteed cure since endometrial-like tissue can still grow outside the uterus.
Many patients struggle to access proper surgical care due to a lack of awareness among doctors, insurance barriers, or being misdiagnosed for years. That’s why seeking an endometriosis specialist is crucial when considering surgical options.
Lifestyle and Alternative Management Strategies
Many people turn to lifestyle changes and alternative therapies to manage their symptoms—often in combination with medical treatments.
Diet and Nutrition
- Some individuals find relief with an anti-inflammatory diet, which includes:
- Leafy greens, berries, and omega-3-rich foods (salmon, flaxseeds).
- Avoiding processed foods, excessive caffeine, and refined sugar.
- Reducing or eliminating gluten, dairy, and red meat may help some people, though research is still ongoing.
Pelvic Physical Therapy
- Chronic pelvic pain can cause tightness and muscle imbalances.
- Pelvic floor therapy can help reduce pain by releasing trigger points and improving mobility.
- Helps with painful intercourse and bladder dysfunction.
Acupuncture and Holistic Approaches
- Some individuals report symptom relief with acupuncture, as it may help reduce inflammation and improve blood circulation.
- Yoga, meditation, and breathwork can help manage stress, which may worsen pain symptoms.
Endometriosis is complex, and no two cases are exactly alike. Some individuals may find hormonal treatments effective, while others struggle with side effects. Surgery may work for some, but not everyone.
That’s why a personalized approach—one that combines medical, lifestyle, and alternative therapies—is often the best way to manage endometriosis. What’s most important is finding a treatment plan that works for you and being an advocate for your own health.

Advocacy and Support for Endometriosis
March is National Endometriosis Awareness Month, a time to unite, educate, and advocate for those affected by endometriosis. Your voice and actions can make a significant impact in raising awareness and driving change. Here’s how you can get involved:
Share Your Story
Personal experiences are powerful tools for awareness. By sharing your journey, you can help others understand the realities of living with endometriosis and foster a supportive community.
- Social Media: Use platforms like Instagram, Twitter, and Facebook to share your story. Include the hashtag #EndometriosisAwareness to connect with a broader audience and amplify your message.
- Blogs and Vlogs: Consider writing a blog post or creating a video detailing your experience. Personal narratives can provide comfort to others facing similar challenges and educate those unfamiliar with the condition.
Participate in Events and Support Research
Engaging in events and supporting research initiatives are tangible ways to contribute to the cause.
- Attend or Organize Events: Participate in local or virtual events such as walks, seminars, or workshops. Organizations like the Worldwide EndoMarch host annual events to raise awareness. Consider organizing your own event to educate your community.
- Donate: Financial contributions to research foundations can accelerate the discovery of better treatments and, ultimately, a cure. The Endometriosis Foundation of America is one such organization dedicated to advancing research and education.
Advocate for Policy Changes
Systemic change is crucial for improving the lives of those with endometriosis.
- Contact Legislators: Reach out to your local and national representatives to express the need for increased funding for endometriosis research and improved healthcare policies.
- Support Advocacy Groups: Align with organizations that lobby for policy changes. The Endometriosis Association offers resources and avenues for advocacy.
Resources and Support Groups
Connecting with others provides emotional support and valuable information.
- The Endometriosis Network Canada: Offers virtual support groups and educational resources. Visit their website at https://endometriosisnetwork.com/.
- Endometriosis Foundation of America: Provides patient support, education, and advocates for research. Learn more at https://www.endofound.org/.
- Endometriosis Association: Focuses on support, education, and research facilitation. Access their resources at https://endometriosisassn.org/.
- Worldwide EndoMarch: A global movement to raise awareness and advocate for those with endometriosis. Find events and information at https://endomarch.org/.
By sharing your story, participating in events, advocating for change, and connecting with support networks, you contribute to a future where endometriosis is better understood and those affected receive the care and recognition they deserve.
Endometriosis is more than just painful periods—it’s a chronic condition that affects millions of people worldwide, yet it remains misunderstood, misdiagnosed, and underfunded. National Endometriosis Awareness Month serves as a reminder that we need to break the silence, push for better healthcare, and support those living with this condition.
If you or someone you love is experiencing symptoms like chronic pelvic pain, heavy periods, painful intercourse, or digestive issues, don’t ignore them. Listen to your body, trust your instincts, and seek medical advice—even if it means getting a second (or third) opinion. Early diagnosis and proper management can make a huge difference.
The more we speak up, share our stories, and advocate for change, the closer we get to a world where endometriosis is recognized, understood, and properly treated. You can be part of the movement by:
- Sharing this post and spreading awareness on social media using #EndometriosisAwareness.
- Joining advocacy efforts to push for better research and healthcare policies.
- Educating yourself and others about the signs, symptoms, and available treatments.
Want to stay informed about endometriosis research, wellness tips, and health advocacy updates? Sign up for our newsletter today and get the latest updates straight to your inbox!
Together, we can bring endometriosis out of the shadows and into the conversation—because no one should have to suffer in silence.

Leave a Reply
You must be logged in to post a comment.