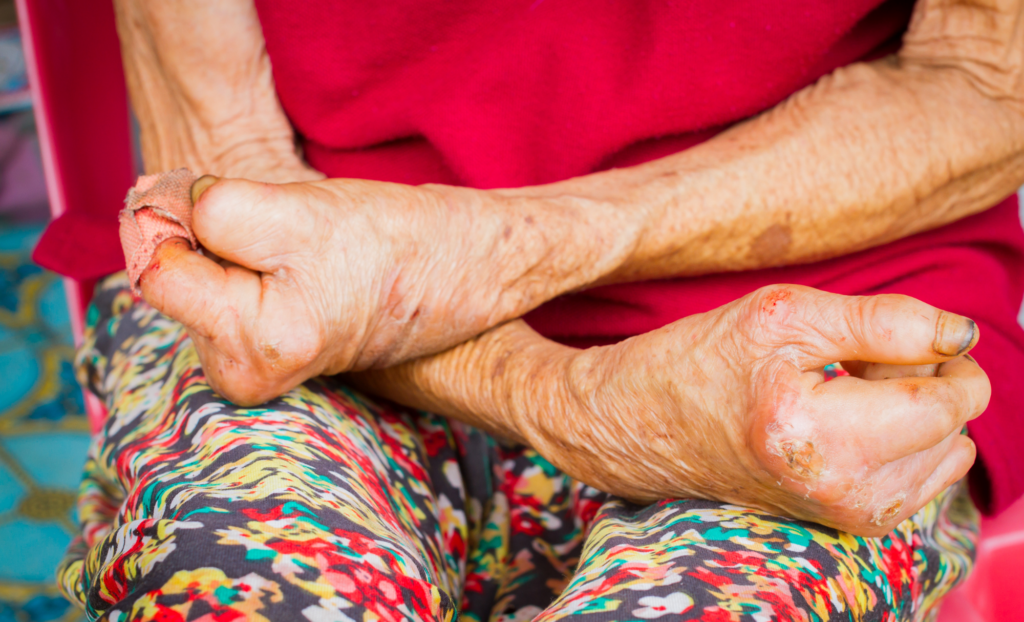
Leprosy, once feared as a curse or a punishment, remains one of the most misunderstood diseases in the world. Despite being one of the oldest known diseases, with historical references dating back thousands of years, leprosy is still a major health issue in certain parts of the world. Every year, World Leprosy Day is observed to raise awareness, reduce stigma, and educate the public about this treatable condition.
While leprosy may not be a widespread concern in many parts of the world today, millions of people still suffer from its effects, particularly in areas with limited access to healthcare. The good news is that leprosy is both treatable and preventable. Early detection and appropriate treatment can prevent the worst complications and help individuals live full, healthy lives.
In this post, we’ll explore what leprosy is, how it’s transmitted, its symptoms, treatment options, and how we can work together to prevent and ultimately eradicate it.
What is Leprosy?
Leprosy, also known as Hansen’s disease, is a chronic infectious disease caused by the bacterium Mycobacterium leprae. It primarily affects the skin, peripheral nerves, upper respiratory tract, and eyes, and can lead to permanent nerve damage and disability if left untreated. While the disease is often associated with physical deformities, it is important to note that leprosy is curable with the right treatment.
Historically, leprosy has been shrouded in stigma, often leading to fear and discrimination against those diagnosed with the disease. In ancient times, people believed it to be highly contagious and associated it with divine punishment. This misconception contributed to the isolation and mistreatment of people with leprosy, even though it’s now known that the disease is not easily spread.
Leprosy is not highly contagious, and transmission is thought to occur through respiratory droplets, particularly from prolonged contact with an untreated person. However, only a small percentage of people who are exposed to the bacteria will actually develop the disease, as most have a natural immunity to it.
In modern times, leprosy is treatable and no longer the deadly or debilitating condition it once was. With the advent of multi-drug therapy (MDT), leprosy can be cured, and patients can live healthy, normal lives. The key to ending the disease lies in early diagnosis, effective treatment, and public education to combat the stigma surrounding it.
Leprosy Symptoms
Leprosy can be difficult to detect in its early stages, as its symptoms develop gradually and may resemble other skin conditions. However, recognizing the signs early is critical for prompt treatment and preventing long-term damage. Symptoms of leprosy primarily affect the skin, nerves, and sometimes the eyes, leading to a range of visible and sensory changes.
Skin Lesions
One of the most noticeable symptoms of leprosy is the appearance of discolored patches or lesions on the skin. These lesions are often lighter or darker than the surrounding skin and may appear flat or raised.
- Loss of sensation: The affected skin areas may become numb, which can lead to injuries or burns that go unnoticed by the patient.
Nerve Damage
Leprosy attacks the nerves, particularly those near the skin. This can lead to numbness, tingling, or weakness in the affected areas, which may include the hands, feet, or face.
- Loss of sensation: This is a hallmark sign, often affecting the extremities, and it can increase the risk of injury, as the patient is unaware of cuts or burns.
- Muscle weakness: As nerves are damaged, muscles may weaken, leading to difficulty in movement and sometimes deformities in the hands or feet.
Eye Problems
In some cases, leprosy can affect the eyes, leading to vision problems and even blindness if left untreated.
- Dry eyes: This can cause irritation and lead to damage to the cornea.
- Blinking difficulties: Damage to the nerves that control eye muscles may result in the inability to blink, which can lead to dryness and injury to the eye.
Progressive Deformities
If leprosy is not diagnosed and treated early, it can lead to deformities due to nerve damage. These can include:
- Claw hand: Caused by muscle weakness and loss of sensation, leading to the curling of fingers.
- Foot drop: Loss of muscle function in the foot, making it difficult to lift the foot while walking, often resulting in dragging the foot.
- Facial deformities: The loss of sensation and nerve damage in the face can lead to changes in facial features, such as the collapse of the nose or earlobes.
Other Signs
- Fatigue and general weakness: These symptoms are often seen in individuals with more advanced cases of leprosy.
- Swollen nerves: Pain or swelling in areas where nerves are affected, such as in the arms or legs.
Early detection of leprosy is key to preventing irreversible nerve damage and disabilities. While leprosy can cause significant physical and sensory damage if untreated, it is curable with multi-drug therapy (MDT), and most people who start treatment early recover fully. Recognizing the symptoms early and seeking treatment is crucial in limiting the impact of the disease.

Causes of Leprosy
Leprosy is caused by the bacterium Mycobacterium leprae, which primarily affects the skin, nerves, upper respiratory tract, and eyes. Although leprosy is not highly contagious, it can spread through prolonged close contact with an untreated individual, particularly through respiratory droplets.
How Leprosy Spreads
Leprosy is thought to be transmitted through droplets from the nose and mouth when an infected person coughs or sneezes. However, the exact method of transmission is still not fully understood, as many people who are exposed to the bacteria do not develop the disease. This suggests that genetic immunity and other factors may play a role in whether or not an individual contracts leprosy.
Unlike some other infectious diseases, leprosy requires prolonged exposure to an untreated person for transmission to occur. It is not spread through casual contact, such as shaking hands or touching surfaces. It is also not passed through sexual contact, as is the case with some other diseases.
The Role of the Immune System
Not everyone who is exposed to Mycobacterium leprae will develop leprosy. In fact, most people who are exposed to the bacteria have a natural immunity to it. This suggests that the body’s immune system plays a crucial role in determining whether leprosy will develop.
While a healthy immune system can fight off the bacteria, those with weakened immune systems or genetic predispositions may be more susceptible to developing leprosy. In these individuals, the bacteria multiply in the body and begin to cause the characteristic symptoms, including skin lesions and nerve damage.
Global Prevalence and At-Risk Populations
Leprosy is most common in areas with tropical and subtropical climates, where access to healthcare may be limited. India, Brazil, and Indonesia are among the countries with the highest number of reported cases.
- Poverty and crowded living conditions increase the risk of transmission, as they can lead to prolonged close contact with untreated individuals.
- People living in rural areas with limited healthcare access may also face higher risks due to delayed diagnosis and treatment.
Leprosy is now rare in most developed countries due to advances in healthcare, early detection, and effective treatments. However, it remains a significant concern in certain regions, especially where healthcare infrastructure is lacking.
Understanding how leprosy spreads and why some people are more vulnerable than others helps reduce the stigma surrounding the disease. Leprosy is not highly contagious and cannot be easily transmitted, which is a critical point to highlight in awareness efforts. Early diagnosis, treatment, and public education are essential in stopping its spread and supporting those affected.
Leprosy Treatment Options
Leprosy is a treatable disease, and with the right medical intervention, patients can recover fully and lead normal lives. The key to effective treatment is early detection and comprehensive care, which can prevent serious complications like nerve damage and physical deformities. Thankfully, advances in medical care have made leprosy curable and manageable for those who seek treatment promptly.
Multi-Drug Therapy (MDT)
The cornerstone of leprosy treatment is Multi-Drug Therapy (MDT), which involves a combination of antibiotics that work together to kill Mycobacterium leprae, the bacteria that causes leprosy. MDT is the standard treatment globally and has been highly effective in reducing the number of active cases of leprosy.
- Drugs involved: MDT typically includes a combination of dapsone, rifampicin, and clofazimine.
- Duration of treatment: Depending on the severity of the disease, treatment typically lasts from 6 months to 2 years.
- Effectiveness: MDT effectively kills the bacteria and prevents further transmission. Once treatment begins, the patient is no longer contagious, allowing them to lead a normal life while undergoing therapy.
Managing Nerve Damage and Complications
One of the primary concerns with leprosy is the nerve damage it can cause, which may lead to loss of sensation, muscle weakness, and deformities. Even after the bacteria are eradicated, some of these complications may remain, requiring ongoing care.
- Pain management: For those suffering from nerve pain, medications such as analgesics or corticosteroids can help manage discomfort.
- Physical therapy: This is often used to improve mobility and prevent deformities, particularly for those with nerve damage in the hands, feet, or face.
- Surgical interventions: In cases of severe deformities or nerve damage, surgery may be required to restore function or improve appearance.
Follow-Up Care and Monitoring
After completing the course of MDT, patients should receive regular follow-up care to ensure that the infection is fully eradicated and to monitor for any side effects of treatment.
- Regular check-ups: These are essential to assess the effectiveness of the treatment and detect any potential relapses early.
- Supportive care: This includes managing side effects of the medication, providing emotional support, and ensuring that patients receive any additional treatments for complications that may arise, such as nerve damage or infections.
Preventing Relapse
Although relapse is rare, some individuals may experience a return of symptoms after completing MDT, especially if treatment was not completed properly.
- Importance of completing treatment: It’s crucial that patients adhere to the full course of MDT to ensure that the bacteria are completely eliminated from the body.
- Monitoring for signs of relapse: Regular follow-up appointments are essential to detect and address any recurrence of symptoms before they cause significant harm.
Addressing Stigma and Providing Support
- Psychosocial support: It’s essential that patients receive counseling and support to help them cope with the psychological and social impacts of leprosy, particularly if they’ve experienced discrimination or isolation.
- Reducing stigma: Community education and awareness campaigns can help reduce the stigma surrounding leprosy and encourage people to seek treatment early without fear of discrimination.
Early and effective treatment with MDT not only helps cure leprosy but also prevents complications such as nerve damage, disabilities, and disfigurement. Thanks to advances in treatment and global efforts to increase awareness, leprosy is no longer the debilitating condition it once was. By continuing to promote early diagnosis and accessible treatment, we can ensure that more people with leprosy recover fully and lead healthy lives.
Leprosy Prevention
Leprosy is a preventable and treatable disease, and efforts to stop its spread can make a significant difference in reducing its impact globally. While there is no specific vaccine for leprosy, there are several effective strategies to prevent new cases and limit transmission.
Early Diagnosis and Treatment
The most effective way to prevent the spread of leprosy is early detection and prompt treatment. The disease is highly treatable with multi-drug therapy (MDT), which is a combination of antibiotics that kill the bacteria causing the disease. Once treatment begins, leprosy is no longer contagious, and patients can live healthy, normal lives. Early treatment also prevents the development of serious complications, such as nerve damage and deformities.
Healthcare workers play a critical role in identifying symptoms early and providing timely access to MDT. Regular screenings in endemic areas can help detect leprosy before it progresses and spreads further.
Improving Access to Healthcare
Improving access to healthcare services is a crucial part of leprosy prevention. In many parts of the world, particularly in rural or impoverished areas, healthcare resources are limited. People in these communities may not seek medical help until the disease has already caused significant damage.
- Mobile health clinics and outreach programs are essential for reaching remote populations and providing education, screening, and treatment.
- Community health workers can help raise awareness, reduce stigma, and encourage early medical intervention.
Reducing Stigma and Increasing Awareness
One of the biggest challenges in preventing leprosy is the stigma that surrounds the disease. Due to misconceptions about leprosy’s contagiousness and its association with social isolation, many people delay seeking medical help until the disease is more advanced.
- Public education campaigns are key in dispelling myths about the disease, especially regarding its low risk of transmission and the fact that it is curable.
- Support for individuals affected by leprosy helps reduce social stigma and encourages others to seek treatment.
Enhanced Sanitation and Living Conditions
Leprosy is most commonly found in tropical and subtropical regions where crowded living conditions and poor sanitation can increase the spread of bacteria.
- Improved living conditions, access to clean water, and better sanitation can help reduce the risk of transmission.
- Better nutrition also plays a role in strengthening the immune system and reducing susceptibility to infections, including leprosy.
Ongoing Research and Development
While MDT has made great strides in treating and curing leprosy, there is ongoing research into developing a vaccine and further improving the treatment regimen.
- Research into vaccination is crucial for long-term leprosy eradication efforts.
- Advances in genetic studies and immune system research can also help identify individuals at higher risk, allowing for earlier intervention.
Leprosy may not be as widespread as it once was, but it still presents a significant health challenge in certain parts of the world. By focusing on prevention—through early diagnosis, treatment, better healthcare access, reducing stigma, and improving living conditions—we can significantly reduce the global burden of leprosy and work toward eradicating it entirely.
Leprosy is a disease that, while still affecting millions in certain parts of the world, is both treatable and preventable. With early diagnosis and the use of multi-drug therapy (MDT), patients can live healthy, productive lives without the debilitating effects that once came with this condition. However, the key to eradicating leprosy is education, awareness, and a commitment to reducing the stigma that has historically surrounded the disease.
As we observe World Leprosy Day, it’s a reminder that we all have a part to play in the fight against leprosy, whether through spreading awareness, supporting those affected, or encouraging early diagnosis and treatment. By learning more about leprosy and supporting efforts for its prevention and treatment, we can make a tangible difference in the lives of those impacted.
Stay informed and continue to learn more about important health topics like leprosy by signing up for our newsletter. You’ll receive regular updates, health tips, and insights that help you stay engaged in the fight to improve global health and wellness.

Leave a Reply
You must be logged in to post a comment.